What is Periodontal Disease?
Periodontal disease (advanced gum disease) is a chronic inflammatory condition affecting the supporting structures of teeth, including gums, periodontal ligament, and alveolar bone.
It’s primarily caused by plaque accumulation that hardens into calculus (tartar) if not removed.
The disease progresses from gingivitis (gum inflammation) to periodontitis, which can lead to irreversible damage such as bone loss and tooth loss.
Symptoms of Periodontal Disease
Early Stage (Gingivitis):
- Red, swollen, or tender gums
- Bleeding during brushing or flossing
- Persistent bad breath (halitosis)
Moderate to Advanced Stage (Periodontitis):
- Receding gums or teeth appearing longer
- Loose or shifting teeth
- Pain while chewing
- Pus between teeth and gums
- Deep periodontal pockets
- Bone loss
Causes of Periodontal Disease
The primary cause is poor oral hygiene, allowing plaque to accumulate. Other contributing factors include:
-
Lifestyle factors: Smoking, poor diet, stress
-
Systemic conditions: Diabetes, cardiovascular disease, autoimmune disorders
-
Hormonal changes: Pregnancy, puberty, menopause
-
Medications: Drugs reducing saliva flow (antihistamines, antidepressants)
-
Genetic predisposition: Family history
Diagnosis Methods
A dentist diagnoses periodontal disease through:
-
Clinical examination: Assessing gum health, measuring pocket depth, checking for bleeding
-
X-rays: Evaluating bone loss around teeth
-
Periodontal probing: Using a calibrated probe to measure periodontal pocket depth
Treatment Options
Treatment depends on severity:
-
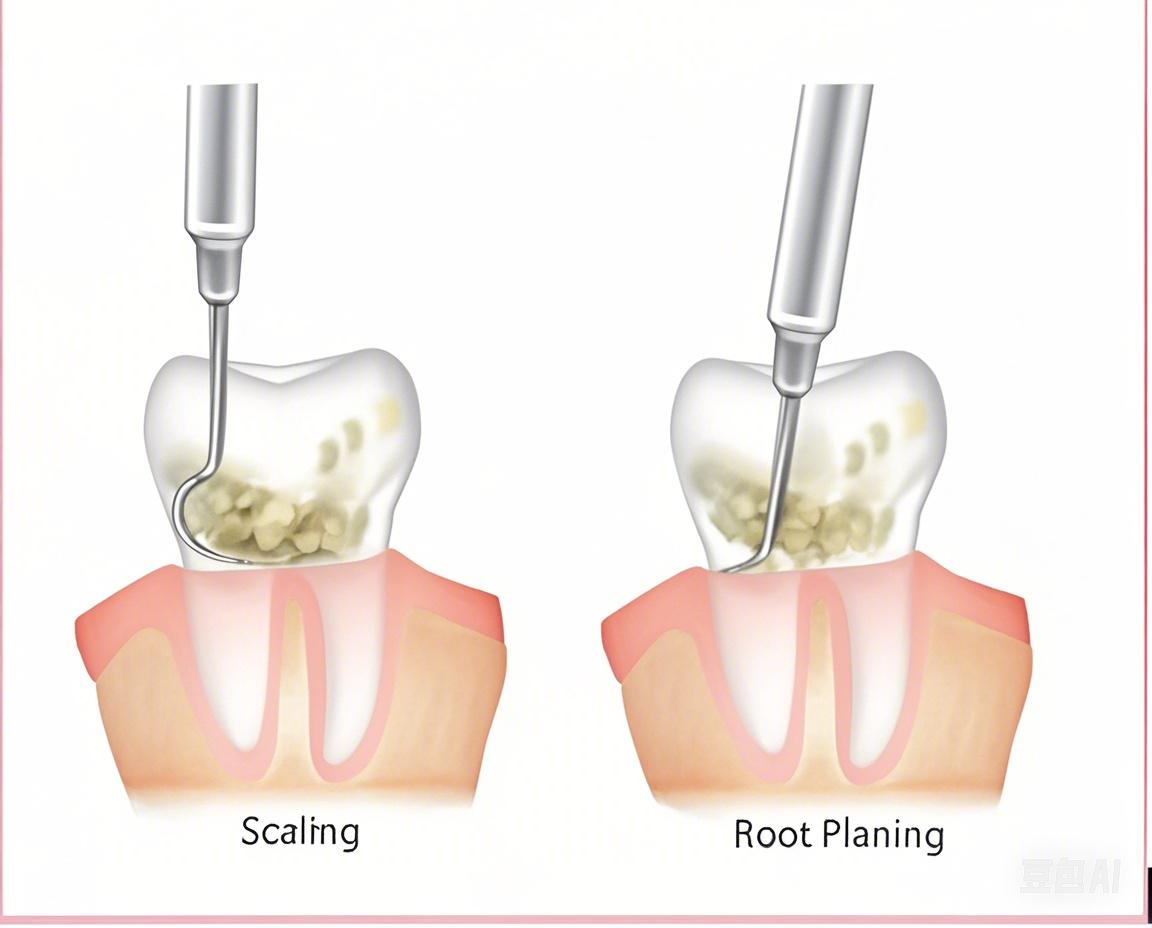
Scaling and Polishing: For mild cases, removes plaque and calculus above and below gum line
-
Root Planing (Deep Cleaning): For moderate cases, smooths root surfaces to remove bacteria
-
Surgical Treatment: For severe cases, may include flap surgery, bone grafting, or guided tissue regeneration
Difference between scaling and root debridement (深層清潔)
Scaling removes plaque and calculus from tooth surfaces.
Root debridement involves more thorough cleaning of root surfaces to remove bacterial toxins and infected tissue to promote healing and gum reattachment.
FAQs About Periodontal Disease
1. Can periodontal disease be prevented?
Yes, through:
-
Brushing twice daily with soft-bristled toothbrush and fluoride toothpaste
-
Flossing daily to remove plaque between teeth
-
Regular dental check-ups every 6-12 months
-
Using antibacterial mouthwash to reduce bacteria
-
Avoiding smoking and managing conditions like diabetes
2. Is periodontal disease reversible?
Gingivitis is reversible with proper treatment and improved oral hygiene. However, periodontitis can only be managed to prevent further damage, as lost bone and tissue cannot fully regenerate.
3. How does periodontal disease affect overall health?
Periodontal disease is linked to:
-
Diabetes: Makes blood sugar control harder; diabetes increases infection risk
-
Cardiovascular disease: Bacteria can enter bloodstream, contributing to arterial plaque
-
Respiratory infections: Inhaling oral bacteria can lead to lung infections
-
Pregnancy complications: Associated with preterm birth and low birth weight
4. Is periodontal treatment painful?
Most treatments use local anesthesia to minimize discomfort.
After treatment, patients may experience mild sensitivity, soreness, or swelling that typically subsides within days. Pain management medications can help.
5. Can I treat periodontal disease at home?
While good oral hygiene is essential, professional treatment is necessary for removing calculus from deep pockets. Home care alone cannot address advanced periodontal disease.
6. How long does periodontal treatment take?
Non-surgical treatments like scaling and root planing can be completed in 1-2 sessions.
Surgical treatments may require multiple visits.
Regular follow-ups are essential to monitor progress.
7. What happens if periodontal disease is left untreated?
Untreated disease can lead to:
-
Severe gum recession and bone loss
-
Tooth loosening and eventual tooth loss
-
Chronic pain and difficulty chewing
-
Increased risk of systemic health issues